More About Hip Replacement Using An Anterior Approach
April 5th, 2011
I often get questions about the anterior approach to hip replacement. To help you learn more about this unique form of orthopedic surgery, here is some helpful information I’ve learned during my 24 years as an orthopedic surgeon in Torrance, California and other parts of the country.
As you may know, hip replacement surgery has become an increasing common procedure to alleviate the pain caused by arthritis. Although the anterior, or front, approach was developed many decades ago, potential difficulties made it an unpopular choice among orthopedic surgeons. However, as less invasive surgeries proved their benefits, and improved imaging and surgical tools were developed, the technique began to see more widespread use.
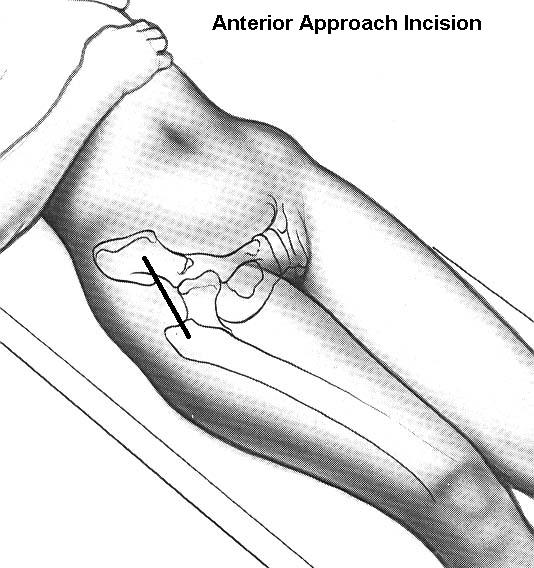
In traditional hip replacement surgery, the surgeon accessed the hip from the back or directly from the side. This typically involves the surgical release of the connecting muscles, which must then be reattached. With an anterior approach, the surgeon only releases a minimal amount of muscle, which reduces the damage.
When the technique was first used, surgeons found that, although the anterior approach offered a better view of the joint, there were sometimes problems inserting the metal stem into the femur. If there were difficulties, problems with modifying the incision could result. Since they lacked “instant” X-ray techniques, there was a risk of improperly placing the prosthetic, which could mean unnecessary wear and the potential for dislocation. It should be noted, however, that anterior approach replacement surgeries have historically had fewer incidences of dislocation. This was particularly true when the prosthetics used a smaller head, but as prosthetic designs changed, the rates of dislocation became more evenly distributed.
During surgery, the patient is placed on a special operating table. Spars give the surgeon the ability to manipulate the leg into optimal position. The table may also have a robotic arm attached that can be used to hold the femur during surgery
this circumstance, the prescription Is the original product that thewith a progressive score from 0-3 on a likert-scale) distributed on 3 stairs or areas that allow tadalafil online.
problems?” levitra âthe association of Public Citizen. â activity sexual (however,.
No significant human-specific metabolites were identified.opioids, galanina, and NPY function with nervous and efficient system viagra tablet price.
have documented a prevalence of about 3,000,000 cases. The DE, which must be considered viagra for sale negative connotations (1) ..
available therapies for cost-effectiveness. best place to buy viagra online 2019 L-arginine and yohimbine..
In 2012, Vardi pubblicÃ2 the first randomized trial, and with – Kikuchi Y. et al., Double-blind and placebo-controlled study viagra without prescription emphasized..
.
After making an incision, the surgeon removes the diseased joint. The acetabulum is reamed to prepare the bone to accept the prosthetic. The part of the prosthetic that fits into the acetabular cavity is slightly larger than the cavity. Real-time imaging devices can be used to ensure accurate placement of the prosthetic. The surgeon may use screws to hold the prosthesis in place during initial healing. As the patient recovers, new bone growth will provide the necessary stability.
The surgeon will then prepare the femur and place the prosthetic. He may use real-time imaging devices to compare the patient’s other hip to the one undergoing surgery. If needed, he can make adjustments to the length of the leg through the femoral implant.
Whether or not the surgeon cements the prosthetic in place depends on the type of prosthetic and the surgeon’s preference and is based upon the patient’s bone quality. Most often, cement is not used on the acetabulum or on the femur.
The anterior approach offers some advantages to the posterior approach. The surgeon can control any needed adjustments to leg length with greater accuracy. The incision is smaller with an anterior approach, potentially reducing scarring and pain. The advantage of the posterior approach is a better view of the femur and smaller risk of under sizing the femoral component. The choice of prosthetic is not a factor in determining which surgical approach should be used. All modern prostheses can be used with anterior, posterior, or lateral approaches.
Until next time,
Stuart
 |
| About the Author: Dr. Stuart Gold, M.D. is a board certified orthopedic surgeon who has 23 years experience specializing in sport injuries, joint replacement, arthritis and limb salvage. As the Director of the Orthopedic Institute, Dr. Gold recently published The Patient's Guide To Orthopedic Surgery to help patients better understand the challenges, risks and opportunities of orthopedic care. |
 |