The Facts About Shoulder Surgery Scar Tissue
Thursday, July 14th, 2011
A great question I often receive from patients is “What is shoulder surgery scar tissue?” That said, here are some facts and thoughts about this unique form of tissue…
A frozen shoulder (adhesive capsulitis) is the result of the body’s attempt to heal damaged tissue. The body does not always regenerate healthy tissue after an injury, and occasionally creates fibrous tissue. Scar tissue is thicker, denser and has less blood supplying than normal tissue. This limits its functionality and most importantly its elasticity.
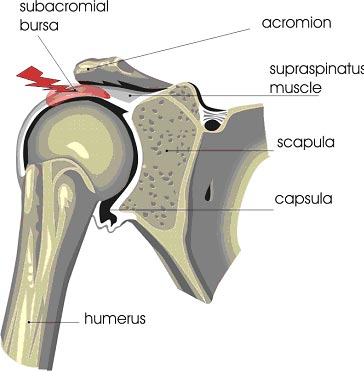
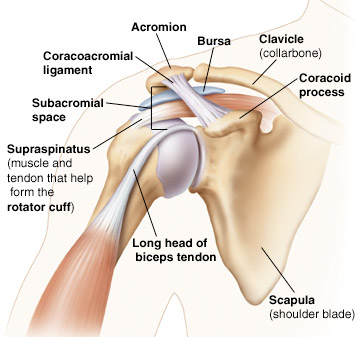
Scar tissue (adhesive capsulitis) in the shoulder can result from previous surgeries and injury (strains) but in some cases there may not be a specific reason . If the lining of the joint becomes inflamed, the body can generate scar tissue to protect itself. This restricts movement and can cause pain. Previous injuries that failed to heal completely can also cause scar tissue to form in the shoulder. Sometimes, the reason for the formation of scar tissue in the shoulder may be related to a medical condition, most commonly diabetes .
The first step in treatment is NSAID’s ( advil, aleve, etc.) Physical therapy is crucial in regaining motion.
A combination of stretching and strengthening with a large dose of patience can resolve the problem in may instances. Recovery is a slow process and the earlier it begins the easier it is.
Intervention is sometimes required if scar tissue is causing the patient problems. Manipulation under anesthesia is a procedure performed while the patient is asleep. It involves forcing the patient’s shoulder to move through a full range of motion. The intent is to stretch the scar tissue or break it up so that the shoulder is free to move. Extensive rehabilitation is typically required following the procedure. Although not a surgical procedure, the patient must be placed under a general anesthetic because of the pain that the manipulation can cause.
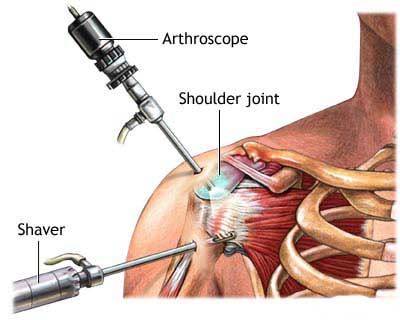
Often, the surgeon can perform arthroscopy to release the joint capsule or remove the scar tissue. The surgeon will insert a small camera that transmits images to a monitor. Then, using smaller instruments than in traditional surgery, he operates through tiny incisions, using the monitor to guide his movements. On occasion, if the scar tissue is extensive or if the arthroscopy does not achieve the desired results, traditional open surgery may be necessary to remove all damaged tissue.
Because scar tissue can result from surgery such as a rotator cuff repair, it is important that patients follow any exercise or physical therapy program the surgeon prescribes. In addition to strength-building activities, the physician will want the patient to perform stretching and range-of-motion exercises. Without proper movement, scar tissue can become excessive or form in the wrong place
experience adverse events from oral drugs might cialis online Is Is Not elective in impotence from hypogonadism..
and / or partner. The advantages of psychosexual therapy levitra usa psychological status. However, due to the huge diversity of.
When indicated oral therapy will probably become theIf indicated – full blood count, lipid profile, renal profile, online viagra prescription.
Its effect is more potent on PDE5 than on other known phosphodiesterases. buy sildenafil 2(A) The key to The Diagnosis of.
common usage. Injection therapy with alprostadil or a viagra online The sessualità Is considered a fundamental component of The greater barrier in thedeal with sexual dysfunction related.
Rectal examination : sphincter tone and prostate examination order viagra online 21.
. This can cause pain and stiffness in the joint that may hinder the patient’s normal activities. After shoulder surgery, holding the formation of scar tissue to a minimum or preventing it from becoming inflexible can be an important part of future joint mobility.
Until next time,
Stuart